Definitions:
- Treated and released emergency department visits: Includes non-fatal emergency department visits that did not result in immediate transfer to a hospital stay.
- Hospitalization: Refers to non-fatal hospital stays, including non-fatal emergency department visits that result in immediate transfer to a hospital stay.
Refer to Appendix 4, Analytic Notes, for more technical documentation.
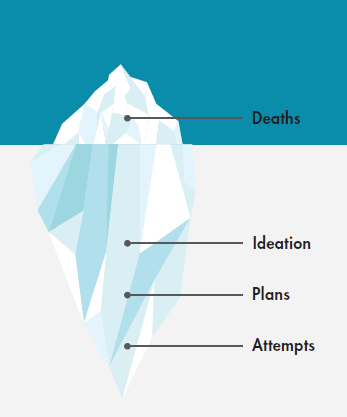 It is important to recognize the broader picture when examining the impact of suicide in our communities. Suicide deaths, while representing tremendous loss, represent a small proportion of the numbers of individuals who experience suicidal thoughts and self-harm behavior. Evidence-based strategies and best practices to prevent suicide should be directed across the full spectrum of behaviors and life events that are associated with suicide risk. For example, a review of emergency department and hospitalization data, which includes people who are treated and released from emergency departments or hospitalization stays with self-harm injuries, illustrates a broader impact of suicide in our communities.
It is important to recognize the broader picture when examining the impact of suicide in our communities. Suicide deaths, while representing tremendous loss, represent a small proportion of the numbers of individuals who experience suicidal thoughts and self-harm behavior. Evidence-based strategies and best practices to prevent suicide should be directed across the full spectrum of behaviors and life events that are associated with suicide risk. For example, a review of emergency department and hospitalization data, which includes people who are treated and released from emergency departments or hospitalization stays with self-harm injuries, illustrates a broader impact of suicide in our communities.
The following data on self-harm injuries presented in this report comes from hospital and emergency department visit records based on codes from the ICD-10-CM. (International Classification of Diseases, 10th Revision, Clinical Modification. See Analytic Notes in Appendix 4.) Emergency department visit data includes only non-fatal, treated and released visits. Hospitalization data includes only non-fatal hospital stays.
In Wisconsin, the age-adjusted rate of emergency department visits with self-harm injuries was 69.6 per 100,000, accounting for 7,482 visits from 2016–2017. The age-adjusted rate of hospitalization with self-harm injuries was 85.3 per 100,000, accounting for 9,398 admissions during the same time period.
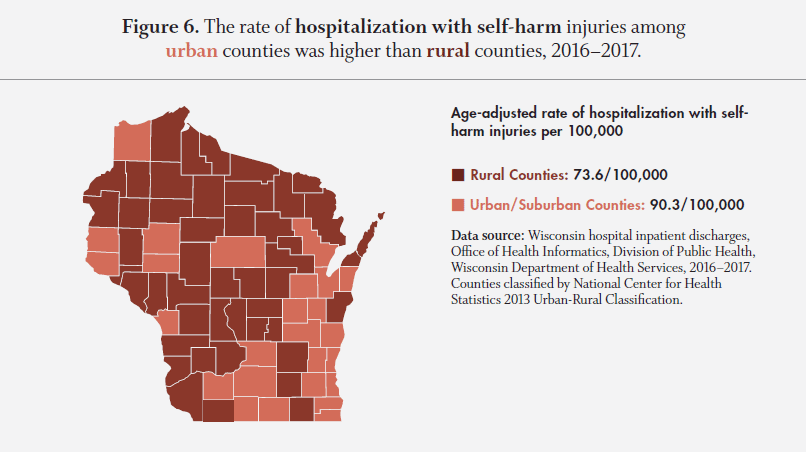
Figure 6. Urban counties had a significantly higher rate of hospitalization with self-harm injuries when compared to rural counties from 2016–2017.
For emergency department visits with self-harm injuries, the rate for rural counties was 68.4 per 100,000 and 70.2 per 100,000 for urban counties from 2016-2017. However, these rates were not significantly different. (County rural and urban classification was determined using the National Center for Health Statistics 2013 Urban-Rural County Classification.)